NCLEX prioritization questions are among the most consistently challenging items on the licensing exam — and among the most important to master. Nearly every nursing student who has worked through a practice question bank has encountered a scenario where multiple patients or multiple nursing actions all seem equally urgent, and the question asks them to choose just one. Without a clear, structured framework, these questions become exercises in guessing rather than clinical reasoning.
The good news is that NCLEX prioritization questions are not random. They follow predictable clinical logic rooted in the same frameworks that guide safe nursing practice: the ABCs, Maslow’s hierarchy of needs, the nursing process, and the principles of safe delegation. Once you understand how these frameworks apply to prioritization scenarios on the exam, what felt like an impossible judgment call becomes a systematic, confident clinical decision.
This guide provides a complete strategy for answering NCLEX prioritization questions correctly in 2026. It covers the frameworks you need, how to apply them step by step, how to handle the most common prioritization scenarios, and how to avoid the reasoning errors that cause well-prepared students to select the wrong answer even when they know the content.
Why NCLEX Prioritization Questions Are So Difficult
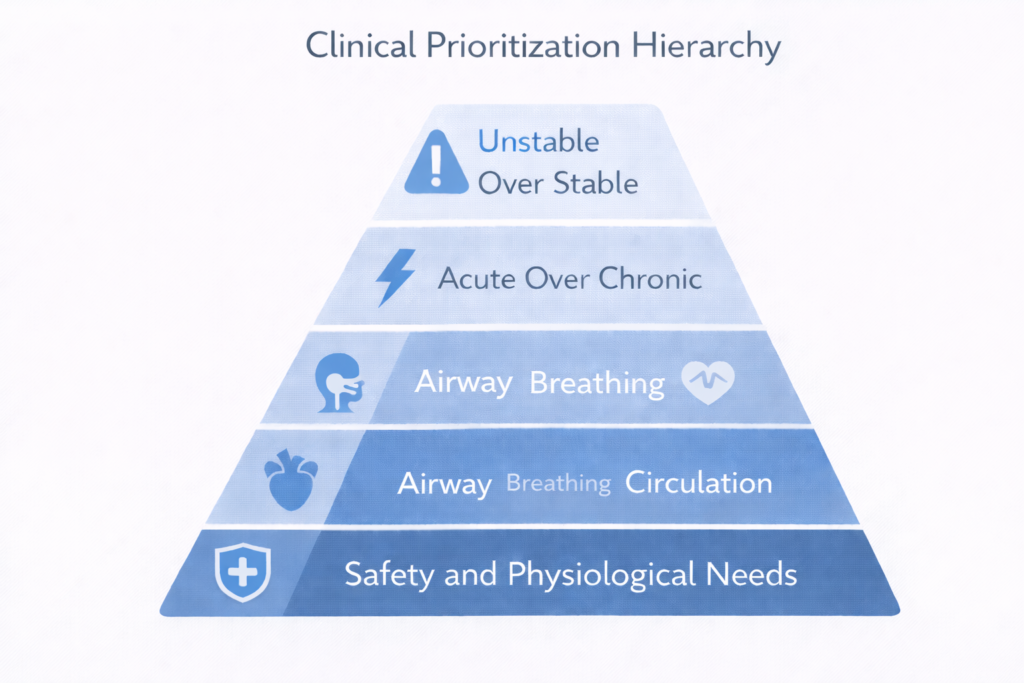
NCLEX prioritization questions are difficult for a specific reason: they are designed to present multiple patients or multiple clinical actions that are all genuinely important, and require you to identify which one is most important right now. The difficulty is not in recognizing that all the options matter — it is in applying the correct clinical hierarchy to determine which one comes first.
Most nursing students are trained to think comprehensively — to address every patient need, to complete every task, to leave nothing unattended. This instinct serves nurses well in clinical practice, where time and resources allow for comprehensive care. But it works against students on NCLEX prioritization questions, where the task is not to do everything but to correctly sequence what gets done first. The shift from comprehensive thinking to hierarchical thinking is the core cognitive skill these questions test.
A second reason NCLEX prioritization questions are challenging is that the wrong answers are rarely wrong because they are bad nursing care. They are wrong because they address a real but lower-priority concern when a higher-priority concern is present. A student who selects a technically correct nursing action but applies it to the wrong patient or at the wrong moment in the clinical sequence will miss the question — not because they did not know what to do, but because they did not correctly identify when to do it.
What Prioritization Questions Are Really Testing
At their core, NCLEX prioritization questions assess your ability to apply the Clinical Judgment Measurement Model’s Prioritize Hypotheses cognitive skill — the ability to rank clinical concerns by urgency and potential harm. The question is always some version of: given everything you know about these patients and this situation, what represents the greatest threat to safety right now, and what must a competent nurse address first?
The Primary Framework: ABCs for NCLEX Prioritization Questions

The ABCs — Airway, Breathing, Circulation — are the foundational framework for NCLEX prioritization questions and should be the first filter you apply to any scenario involving physiological concerns. This hierarchy reflects the order in which physiological compromise becomes life-threatening: an obstructed airway produces unconsciousness and death faster than respiratory failure, which produces deterioration faster than circulatory compromise in most clinical scenarios.
Airway Always Comes First
On NCLEX prioritization questions, any patient with an actual or threatened airway obstruction takes priority over all other patients. Signs of airway compromise include stridor, drooling, inability to speak, facial or neck trauma, a decreasing level of consciousness in a patient who was previously alert, or a known history of anaphylaxis with the onset of throat tightness. When one of the patients in a prioritization scenario presents with any of these findings, that patient is almost always the correct first priority regardless of what is happening with the other patients.
Breathing Is the Second Priority
After confirming that no patient has an airway emergency, evaluate breathing. Patients with acute respiratory distress — severe dyspnea, oxygen saturation below 90 percent, accessory muscle use, cyanosis, or a respiratory rate above 30 or below 10 — take priority over patients with circulatory or other concerns. On NCLEX prioritization questions, a patient in active respiratory distress outranks a patient with chest pain that is not yet causing hemodynamic instability, a patient with a high blood pressure reading without acute symptoms, or a patient with pain that is not compromising breathing.
Circulation Follows Breathing
Circulation concerns — hypotension, tachycardia, active bleeding, signs of shock — take priority over all non-physiological concerns but rank below airway and breathing emergencies. On NCLEX prioritization questions, a patient showing signs of circulatory compromise such as a systolic blood pressure below 90, a heart rate above 130, pallor, diaphoresis, or altered mental status consistent with reduced cerebral perfusion takes priority over a patient with pain, a patient who needs teaching, or a patient with a laboratory value that is abnormal but not acutely dangerous.
The Secondary Framework: Maslow’s Hierarchy for NCLEX Prioritization Questions
When NCLEX prioritization questions involve a mix of physiological and psychosocial concerns — or when all patients are physiologically stable and the question asks which psychosocial or educational need to address first — Maslow’s hierarchy of needs is the correct framework to apply. Maslow’s model ranks human needs from most basic to most complex: physiological needs, safety and security, love and belonging, esteem, and self-actualization.
For NCLEX prioritization questions, the practical application is straightforward: physiological needs always take priority over psychosocial needs. A patient who is experiencing pain, hunger, difficulty breathing, or disrupted sleep has a physiological need that takes precedence over a patient who is experiencing loneliness, anxiety about their diagnosis, or concerns about their role function. Safety needs — the risk of falling, the risk of self-harm, the need for a secure environment — rank just below physiological needs and above all other psychosocial concerns.
When All Patients Are Stable: Applying Maslow to Psychosocial Prioritization
On NCLEX prioritization questions where all patients are physiologically stable, Maslow guides the selection between psychosocial priorities. A patient who is expressing suicidal ideation or a risk of self-harm represents a safety need and takes priority over a patient who needs discharge teaching, a patient who is expressing sadness about their diagnosis, or a patient who wants to talk about their concerns. A patient who has not eaten and is reporting significant hunger has an unmet physiological need that takes priority over a patient who needs emotional support. Apply Maslow consistently and the hierarchy will reliably identify the correct first priority.
Additional Principles for NCLEX Prioritization Questions

Beyond the ABCs and Maslow’s hierarchy, several additional clinical principles help resolve NCLEX prioritization questions when the primary frameworks do not immediately identify a clear winner.
Acute Over Chronic
When comparing two patients with physiological concerns, a patient experiencing an acute change in condition takes priority over a patient with a chronic condition that is at its expected baseline. A patient with chronic heart failure who is currently at their usual weight and activity tolerance is lower priority than a patient who has just developed sudden-onset shortness of breath and diaphoresis. The acute change signals a new, potentially life-threatening development that requires immediate assessment. The chronic stable condition represents a known, managed clinical state that can safely wait.
Unstable Over Stable
Clinical instability — defined as vital signs outside of expected parameters, a declining level of consciousness, a new symptom that represents a departure from the patient’s baseline, or a condition with high potential for rapid deterioration — takes priority over a patient who is stable and whose condition is progressing as expected. On NCLEX prioritization questions, the unstable patient is almost always the correct first priority when comparing patients with different stability levels, even if the stable patient’s underlying condition is more serious in the abstract.
New or Unexpected Findings Over Expected Findings
A new or unexpected clinical finding in a patient always generates higher priority than an expected finding in another patient. A postoperative patient who develops sudden tachycardia and hypotension is higher priority than a postoperative patient who reports incisional pain at a three out of ten — because the tachycardia and hypotension are unexpected and potentially signify hemorrhage, while the mild incisional pain is an expected postoperative finding. On NCLEX prioritization questions, train yourself to identify which patient is experiencing something unexpected, and that patient will almost always be your first priority.
Step-by-Step Strategy for Answering NCLEX Prioritization Questions
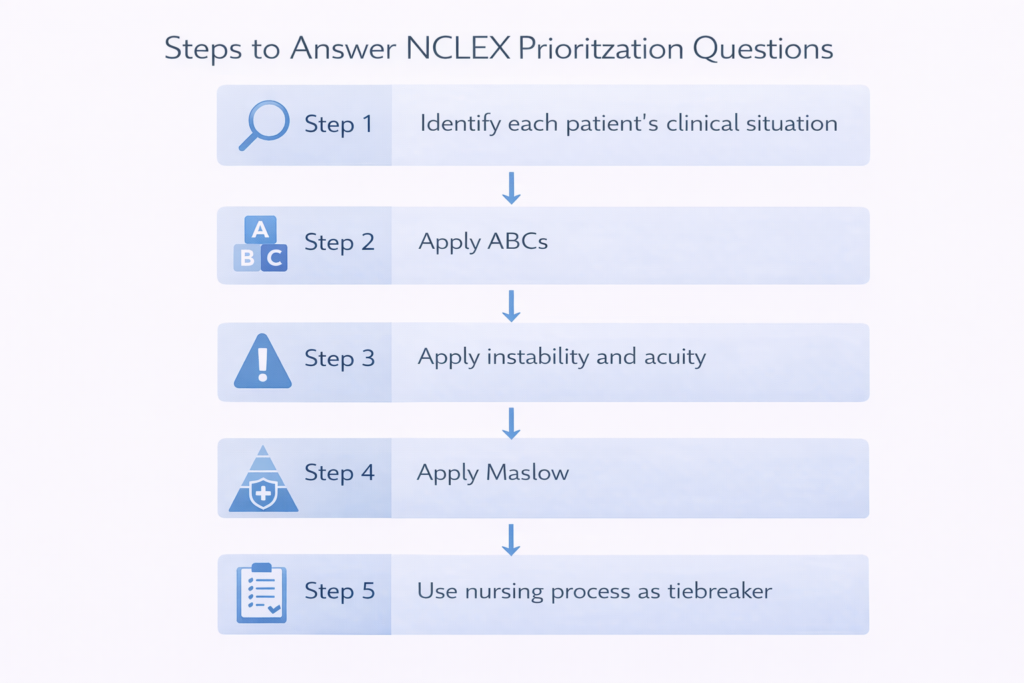
Applying the frameworks above becomes most reliable when you follow a consistent step-by-step process with every NCLEX prioritization question. The following sequence integrates the ABCs, Maslow, and the additional principles into a repeatable decision strategy.
Step 1: Identify What Each Patient or Option Represents
Before applying any framework, read the entire question stem and identify the clinical situation of each patient or option clearly. What is each patient’s primary concern? What are their vital signs? What new or unexpected finding, if any, is present? What is each patient’s trajectory — stable, improving, or deteriorating? Gathering this clinical picture before beginning your prioritization prevents the common error of reacting to surface-level details without understanding the full clinical context.
Step 2: Apply the ABCs First
Scan your patient list for airway or breathing compromise first. If any patient shows signs of airway obstruction or acute respiratory distress, that patient is your priority and your answer is determined. If no patient has an airway or breathing emergency, scan for circulatory compromise — hypotension, tachycardia, active bleeding, signs of shock. If one patient has circulatory compromise and others do not, that patient is your priority.
Step 3: Apply Instability and Acuity If the ABCs Do Not Resolve the Question
If the ABCs do not immediately identify a clear priority — for example, if all patients have stable vital signs — apply the instability and acuity principles. Which patient is experiencing an acute change? Which patient has a new or unexpected finding? Which patient has the greatest potential for rapid deterioration? The answers to these questions will identify the priority patient or action in the majority of remaining scenarios.
Step 4: Apply Maslow for Psychosocial Questions
If the question involves psychosocial concerns or a mix of physical and emotional needs, apply Maslow. Physiological needs rank above safety needs, which rank above all other psychosocial concerns. A patient with an unmet physiological need takes priority over a patient with a safety concern, who takes priority over a patient with an esteem or belonging need.
Step 5: Use the Nursing Process as a Final Tiebreaker
When two options remain equally plausible after applying all frameworks, use the nursing process as a tiebreaker. Assessment precedes diagnosis, which precedes planning, which precedes implementation, which precedes evaluation. If one answer choice involves assessment and another involves intervention, and the clinical scenario has not yet established a clear baseline, the assessment option is typically correct. The NCLEX consistently rewards candidates who gather information before acting.
Common Errors on NCLEX Prioritization Questions and How to Avoid Them
Even students who understand the prioritization frameworks make predictable errors on NCLEX prioritization questions. Recognizing these patterns prevents them from costing you points on exam day.
- Prioritizing based on diagnosis rather than current clinical status: A patient with a serious diagnosis — cancer, heart failure, sepsis — is not automatically the highest priority. Priority is determined by current clinical stability, not diagnosis severity. A patient with a serious diagnosis who is currently stable is lower priority than a patient with a less serious diagnosis who is acutely decompensating.
- Selecting the most active intervention over assessment: On NCLEX prioritization questions that ask what to do first, assessment is almost always the correct first action when the clinical picture is not yet fully established. Students who select a treatment intervention before the scenario has confirmed that the intervention is indicated will consistently miss these questions.
- Ignoring vital signs in the scenario: Vital signs are clinical clues placed deliberately in NCLEX prioritization scenarios. A patient with a respiratory rate of 32, an oxygen saturation of 88 percent, or a blood pressure of 80/50 is telling you exactly where the priority lies. Read every vital sign in the scenario as a clinical signal, not as background detail.
- Applying Maslow when the ABCs apply: Maslow is the framework for psychosocial prioritization when patients are physiologically stable. It does not override the ABCs. A patient with a physiological emergency always takes priority over a patient with even the most significant psychosocial concern.
- Treating all patients as equally urgent: Some students approach prioritization questions by trying to find a reason every patient could be the priority, which leads to decision paralysis. Apply the frameworks systematically and trust the hierarchy. The frameworks exist precisely because not all clinical urgencies are equal.

Conclusion
NCLEX prioritization questions become significantly less intimidating once you have a clear, reliable framework to apply to them. The ABCs identify life-threatening physiological emergencies. Maslow ranks psychosocial needs when patients are stable. Acute over chronic, unstable over stable, and unexpected over expected findings resolve the majority of remaining prioritization decisions. And the five-step strategy ties all of these frameworks into a repeatable, systematic process you can apply to every prioritization scenario you encounter.
Practice these frameworks on every prioritization question in your preparation — not just the ones you find difficult. The goal is to make this reasoning process automatic before exam day, so that when NCLEX prioritization questions appear on the actual exam, you reach for the framework instinctively rather than trying to reconstruct it under pressure. With consistent practice and a clear strategy, prioritization questions become one of your strongest question types rather than your most feared.
What is the best strategy for NCLEX prioritization questions?
The best strategy for NCLEX prioritization questions is to apply a consistent framework hierarchy: start with the ABCs to identify airway or breathing emergencies, then assess for circulatory compromise, then apply instability and acuity principles, then use Maslow for psychosocial questions, and use the nursing process as a final tiebreaker. Applying these frameworks in order systematically resolves the majority of prioritization scenarios.
When do you use Maslow’s hierarchy on the NCLEX?
Use Maslow’s hierarchy on NCLEX prioritization questions when patients are physiologically stable and the question involves choosing between psychosocial needs, or when comparing a psychosocial need to a physiological one. Physiological needs rank above safety needs, which rank above all other psychosocial concerns. Maslow does not override the ABCs — any physiological emergency takes priority over any psychosocial concern.
How do you decide which patient to see first on the NCLEX?
Apply the ABCs first — the patient with airway or breathing compromise is almost always the first priority. If all patients have stable airways and breathing, identify who has circulatory compromise. If all patients are hemodynamically stable, compare acuity: the patient with an acute change, an unexpected finding, or the greatest potential for rapid deterioration takes priority over a stable patient with an expected clinical presentation.
Does acute always beat chronic on NCLEX prioritization questions?
Yes, in the vast majority of NCLEX prioritization questions. An acute change in a patient’s condition represents a new and potentially life-threatening development that requires immediate assessment, while a chronic condition at its expected baseline represents a known, managed clinical state. The exception is when a chronic condition is currently producing an acute physiological emergency — in that case, the ABCs determine priority, not the acute-versus-chronic distinction alone.
What does ‘first’ mean on NCLEX prioritization questions?
‘First’ on NCLEX prioritization questions means the single most important nursing action or the highest-priority patient given the current clinical situation. It does not mean the only action — it means the action or patient that takes precedence over all others at this specific moment. Apply the ABCs and prioritization frameworks to identify what is most acutely life-threatening or most immediately necessary, and that is your first priority.

Leave a Reply